Treating iron deficiency anaemia
The aim of treatment is to replenish iron stores and normalise haemoglobin concentrations.
Dietary therapy
- Increasing dietary intake alone is inadequate to treat iron deficiency anaemia.
- Valuable for primary and secondary prevention of iron deficiency.
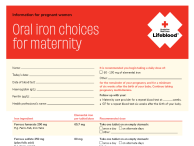
Oral iron therapy
Formulations
- There are more than 100 iron containing preparations available over the counter in Australia but few contain a therapeutic dose for the treatment IDA.
- Multivitamin-mineral supplements should be avoided because the elemental iron content is low (frequently 5 mg or less) and they may contain other ingredients that limit absorption.
- A list of currently available oral preparations for the treatment of iron deficiency anaemia in Australia, with dosing and considerations, can be found here.
Dose
- Oral iron is first-line treatment for most patients and should be continued for three months after normalisation of Hb.
- Historically, 100–200 mg of elemental iron daily in 2 to 3 divided doses have been recommended for adults. Doses as low as 60 mg on alternate days may be effective.
- Doses of 3–6 mg/kg/day of elemental iron are advised for children.
Side effects
Gastrointestinal side effects such as abdominal pain, nausea, vomiting, constipation and diarrhoea are common. Black discolouration of faeces is an expected occurrence.
Strategies to manages these side effects include to:
- take with or shortly after food or at night
- start at a low dose and gradually increase, and/or
- give in smaller doses – either intermediate dose tablets or intermittent dosing (e.g. second daily to weekly).
Teeth discolouration or staining can occur with liquid iron and is best managed by diluting with water and/or drink through a straw. Brushing teeth with baking soda or peroxide may reduce discolouration.
Inadequate response
An inadequate response to oral iron therapy may be due to a number of reasons with more than one factor often involved.
Inadequate iron intake
- Patient not taking oral iron therapy.
- Patient taking an iron supplement or multivitamin tablet with insufficient iron content.
Inadequate iron absorption
- Concomitant consumption of inhibitors of iron absorption (e.g. tea, calcium, antacids, tetracycline, within 2 hours of iron ingestion).
- Coexisting inflammation with functional iron deficiency.
- Intestinal mucosal disorders (e.g. coeliac disease, inflammatory bowel disease).
- Impaired gastric acid secretion (including use of proton pump inhibitors).
- Gastric/intestinal bypass procedures.
- Helicobacter pylori colonisation.
Ongoing iron losses or iron requirement in excess of dose absorbed
- Occult, undiagnosed or recurrent gastrointestinal blood loss (e.g. peptic ulcer, malignancy, angiodysplasia, small bowel lesion, parasites).
- Other source of recurrent blood loss (e.g. menorrhagia due to uterine pathology or an inherited bleeding disorder such as von Willebrand disorder).
- Multiple sources of recurrent blood loss (e.g. hereditary haemorrhagic telangiectasia).
- Ongoing urinary iron losses (e.g. significant valve haemolysis).
- Renal failure responding to erythropoietin-stimulating agents.
Coexisting condition interfering with bone marrow response
- Superimposed infection, inflammation, malignancy or renal failure.
- Concomitant B12 or folate deficiency.
- Coexisting primary bone marrow disease or suppression.
Incorrect diagnosis or more than one cause of anaemia
- Anaemia of chronic disease or renal failure.
- Haemoglobinopathy.
- Other causes of anaemia (e.g. haemolysis, myelodysplastic syndromes, congenital anaemia, endocrine disorders).
- Iron-refractory iron deficiency anaemia (IRIDA) is a recently discovered, rare, autosomal recessive disorder that is unresponsive to treatment with oral iron. It represents less than 1% of the cases of iron-deficiency anaemia seen in medical practice.
Medication and food interactions
Oral iron can interact with various medications and foods. It’s important that clinicians make sure their patients are aware of these possible interactions.
Iron absorption may be increased by
- Chloramphenicol - increases serum iron concentration due to chloramphenicol-induced bone marrow toxicity. Consider stopping chloramphenicol and seek specialist advice.
Iron absorption may be decreased by
- Antacids - separate dosage times by as long as possible.
- Calcium (e.g. in dairy products such as milk) - separate dosage times by several hours.
- Phytates (e.g. whole grain cereals) - separate dosage times by several hours.
- Tea and coffee - separate dosage times by several hours.
Iron may decrease the absorption of
- Oral bisphosphonates (e.g. alendronate, clodronate, etidronate, ibandronic acid, risedronate, tiludronate) - do not take iron within 2 hours of taking an oral bisphosphonate.
- Levodopa, carbidopa - separate dosage times by as long as possible.
- Methyldopa - separate dosage times by 2 hours; monitor BP and adjust methyldopa dose if necessary.
- Penicillamine - give iron at least 2 hours before penicillamine.
- Thyroid hormones (e.g. liothyronine, thyroxine) - separate dosage times by 4–5 hours.
Iron absorption is decreased by and iron decreases the absorption of
- Oral quinolones (e.g. ciprofloxacin, moxifloxacin, norfloxacin) - take quinolone at least 2 hours before iron.
- Tetracyclines (e.g. doxycycline, minocycline) - separate dosage times by as long as possible (at least 2 hours).
Parenteral iron therapy
Intravenous iron
- Indicated where oral iron can’t be used, isn’t effective or poorly tolerated, or where rapid restoration of haemoglobin and iron stores is required to avoid decompensation and subsequent red cell transfusion.
- Increasing evidence for first-line treatment of iron deficiency in patients with complex medical conditions such as:
- Congestive cardiac failure
- Inflammatory bowel disease
- Chronic kidney disease
- Four formulations are currently available in Australia: Iron polymaltose, iron sucrose, ferric carboxymaltose and ferric derisomaltose
- Always refer to local health service guidelines/protocols and product information for the specific iron preparation. Maximum doses, dilution and infusion rates are not interchangeable between the different IV iron preparations.
Intramuscular iron
Although effective, it is discouraged as the injection is painful and may be associated with permanent discolouration.
Blood transfusion
- Sub-optimal identification, investigation and management of IDA can lead to unnecessary and reflex decisions to transfuse. In compensated patients who do not require an immediate increase in oxygen carrying capacity, transfusion carries unnecessary risks and fails to replenish deficient iron stores.
- Red blood cell transfusions are only administered to patients with severe anaemia compromising end-organ function (e.g. angina or cardiac failure) or where IDA is complicated by serious, acute ongoing bleeding.
- Iron therapy should follow to replenish iron stores.
- Evidence-based guidance for clinical decision-making in relation to transfusion can be found in the National Blood Authority Patient Blood Management Guidelines.