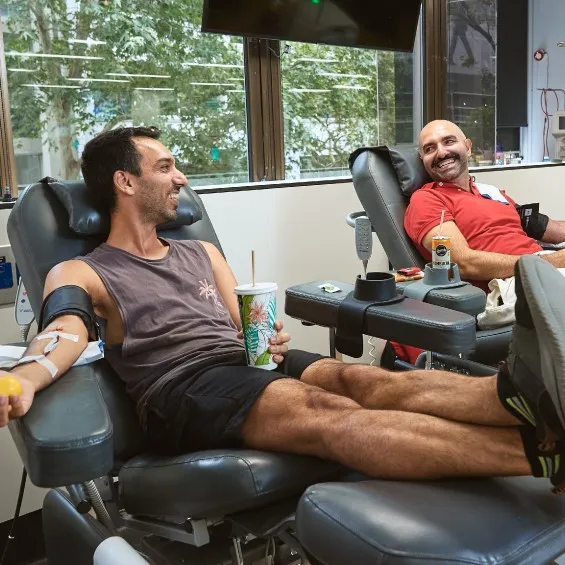
Donation equality
A change for life
Many people who couldn’t donate blood under our previous rules about sexual activity can now give it. And most can donate plasma, too. As long as you meet all our other usual donation criteria, of course.
Let’s get into it.
First of all, most people can donate plasma straight away. No wait period, just changing lives.
As for blood and platelets? You can donate, but you might need to wait a bit if you’ve had sex (excluding oral sex) in the past 6 months with someone new or with more than one person, and you’ve had anal sex in the past 3 months.
For most people in a long-term monogamous relationship, there’s no wait.
So, that means we’ve changed the questions we ask donors so they’re the same for everyone. Regardless of your gender or sexuality. You can see our new questionnaire here.
It’s simple. Fair. Inclusive.
Safety and patients
Patient safety is at the heart of everything we do. Australia even has one of the safest blood supplies in the world. And that isn’t changing. The only thing that is? More people can save lives.